UNT audiology faculty instrumental in providing evidence that led to expanded Medicare coverage for cochlear implants
Dr. Sharon Miller, assistant professor in the College of Health and Public Service Department of Audiology and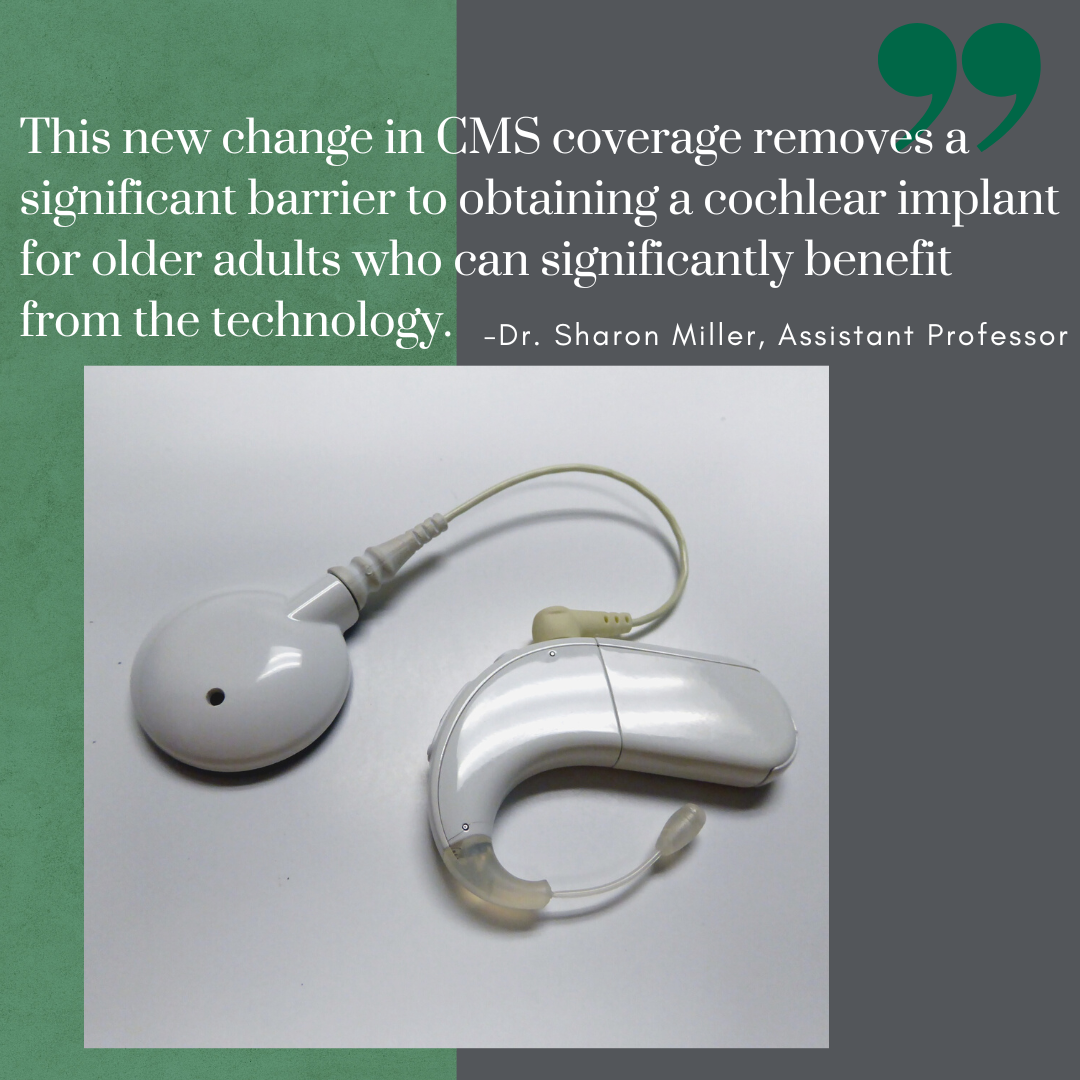 Speech-Language Pathology, was part of a team of researchers whose work led the Centers for Medicare & Medicaid Services (CMS) to update their cochlear implant candidacy criteria to provide coverage for a broader spectrum of hearing loss.
Speech-Language Pathology, was part of a team of researchers whose work led the Centers for Medicare & Medicaid Services (CMS) to update their cochlear implant candidacy criteria to provide coverage for a broader spectrum of hearing loss.
DENTON (UNT), Texas – Dr. Miller was part of the CMS National Coverage Analysis that led to the recommendation that older individuals who receive Medicare benefits with speech test scores of greater than 40% and less than or equal to 60% qualify for cochlear implantation. Previously, only those whose score was below 40% could qualify. The change became effective Sept. 26 and will drastically expand care for older adults with a broader spectrum of hearing loss. Prior to this decision, cochlear implantation was only covered by Medicare for patients who did not meet candidacy criteria when they were enrolled in either a specific type of FDA-approved clinical trial, a trial under the CMS Clinical Trial Policy, or a prospective, controlled comparative trial approved by CMS.
The current decision specifically states: Cochlear implants are an appropriate treatment of bilateral pre- or post-linguistic, sensorineural, moderate-to-profound hearing loss in individuals who demonstrate limited benefit from amplification defined by test scores of less than or equal to 60% correct in the best-aided listening condition on recorded tests of open-set sentence recognition.
“Along with my UNT colleague Dr. Erin Schafer, our research has shown that older adults who receive a cochlear implant obtain significant improvement in speech recognition in quiet and in background noise,” Dr. Miller said. “More importantly, we have also documented significant improvements in overall quality of life because of access to cochlear implants.”
Patients do need to meet other criteria defined by the CMS, such as having limited benefit from appropriate hearing aids, no ear infections or other impediments to the implantation, and no contradictions to surgery.
“Increasing access to cochlear implants is crucial to reduce health disparities related to untreated hearing loss,” Dr. Miller said. “This new change in CMS coverage removes a significant barrier to obtaining a cochlear implant for older adults who can significantly benefit from the technology.”
- Audiology & Speech Language Pathology


